Decoding Hormonal, Circulatory, and Emotional Causes
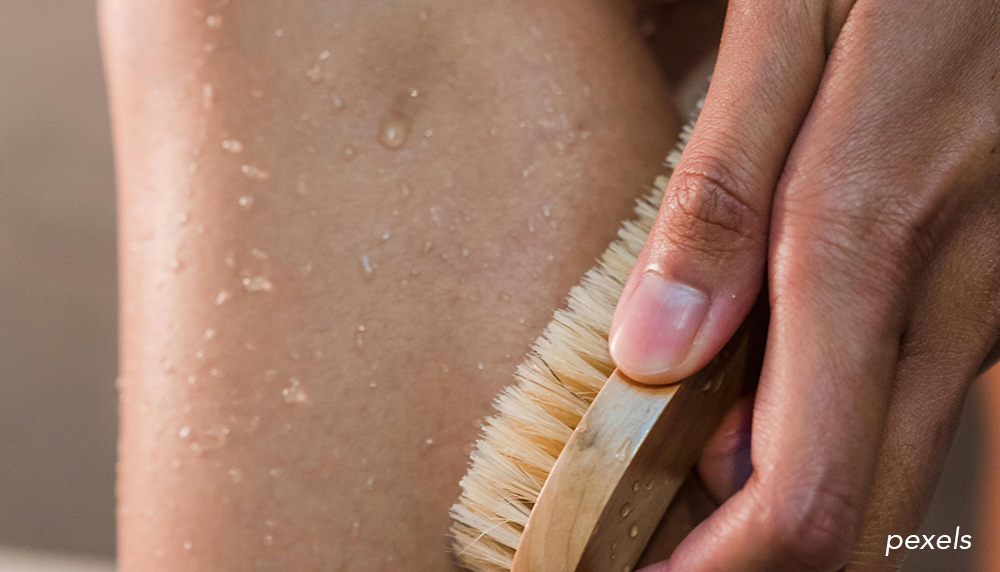
Cellulite and skin. Those familiar small dimples that give the skin an uneven, sometimes “orange peel” appearance , is far more than a simple cosmetic concern. Behind this appearance lies a complex physiological mechanism influenced by multiple factors: hormonal, circulatory, and even emotional. To truly understand this phenomenon, we must go beyond common misconceptions and explore the science behind the skin’s appearance.
Introduction: Why This Article?
Cellulite affects a very large majority of women after puberty: it is estimated to concern between 80% and 98% of them, particularly on the thighs, buttocks, and hips. Despite its prevalence, its exact cause remains complex and multifactorial. It is not a disease, but rather a physiological variation in the distribution of adipose tissue beneath the skin, modulated by several bodily systems. (PMC)
In this article, we will explore three main explanatory axes:
- Hormonal causes
- Circulatory causes
- Emotional and lifestyle-related causes
1. Hormonal Causes: When the Body’s Messengers Shape the Skin
1.1. The Role of Female Hormones
Science shows that hormones play a major role in the appearance of cellulite, especially in women. Among them, estrogen and progesterone are particularly involved:
- Estrogen: These hormones influence fat storage in characteristic areas (thighs, buttocks), promote water retention, and modulate collagen production (the protein that keeps skin firm). (Aesthé)
- Progesterone: Fluctuating during the menstrual cycle, it can encourage water retention and increase pressure on fatty tissues, worsening the dimpled appearance. (Aesthé)
These hormonal variations partly explain why cellulite can intensify at certain times of the cycle, during pregnancy, or during menopause. (Aesthé)
1.2. Other Hormones Involved
Beyond sex hormones:
- Cortisol, the stress hormone, is linked to fat metabolism: excess levels promote collagen breakdown and fat accumulation in certain areas. (Evolys Bien-Être)
- Insulin and thyroid hormones also participate in metabolic regulation and can influence the structure of adipose tissue. (Evolys Bien-Être)
Hormones do not act alone: they interact with other systems in the body and form a complex network that can either amplify or reduce the appearance of cellulite. (Wikipedia)
2. Circulatory Causes: Microcirculation at the Heart of the Phenomenon
If hormones set the stage, blood and lymphatic circulation regulate the local tissue environment, strongly influencing the skin’s appearance.
2.1. Impaired Microcirculation: A Central Clue
Research indicates that microcirculatory disorders , particularly less efficient capillary circulation , are a key factor in the development of cellulite. (MDPI)
Poor circulation means that:
- nutrients and oxygen do not efficiently reach hypodermal cells,
- metabolic waste accumulates,
- and water retention occurs more easily.
This promotes an increase in the volume of adipocytes (fat cells) and their protrusion into the dermis, creating visible irregularities. (MDPI)
2.2. Lymphatic System and Fluid Stagnation
The lymphatic system, responsible for removing fluids and toxins, can become sluggish or inefficient, often due to a lack of physical activity or prolonged sitting. This fluid stagnation leads to water retention, which adds to the visual effect of so-called “watery” cellulite. (EAFIT)
2.3. Arterial, Venous Circulation, and Subtle Inflammation
Altered microcirculation can also generate low-grade micro-inflammation, prolonging or worsening the skin’s appearance. Although cellulite is not inflammation in the classical medical sense, these circulatory difficulties create an environment that favors toxin accumulation and weakening of connective tissue. (Wikipedia)
3. Emotional and Lifestyle-Related Causes: The Brain Influences the Body
3.1. Chronic Stress and the Cascade Effect
Emotional stress , whether related to work, personal life, or body image , is not merely psychological; it has concrete physiological effects. Chronic stress increases cortisol levels, which:
- promote fat storage,
- degraded collagen,
- slow blood circulation. (Evolys Bien-Être)
Thus, accumulated stress can reinforce existing cellulite.
3.2. Sedentary Lifestyle, Diet, and Metabolism
Daily habits play a significant role:
- Sedentary behavior reduces blood and lymphatic flow, promoting stagnation. (EAFIT)
- A diet high in sugars, saturated fats, and salt encourages water retention and subcutaneous fat accumulation. (EAFIT)
- Lack of sleep and poorly managed stress disrupt hormonal balance (notably cortisol and insulin regulation), reinforcing the phenomenon. (Evolys Bien-Être)
3.3. Psychosocial Perspective
Although cellulite is not a disease, it can affect self-esteem and body image and sometimes lead to anxiety or psychological distress. Ironically, these emotional states can sustain a stress cycle that worsens the physiological mechanisms described above. (Wiley Online Library)
4. Why Do All These Causes Interact?
Cellulite is not the result of a single isolated factor; it is the product of a set of biological and environmental interactions. Hormones define a favorable terrain (women are more affected than men), circulation modulates the local tissue environment, and emotional state/lifestyle influences both.
This mechanism explains why some people develop more cellulite than others, even with similar body weight. It also explains why changing a single factor (such as losing weight) is not enough to permanently eliminate cellulite: it is deeply linked to adipose tissue organization, microcirculation, and hormonal balance. (Wikipedia),
Conclusion: Cellulite and skin
Cellulite is far more than a simple cosmetic issue: it reflects a complex interaction between hormones, circulation, and emotional states/lifestyle. Understanding these links not only helps us better understand our own bodies, but also encourages more effective, sustainable, and physiologically respectful strategies.
Rather than viewing it as a “failure” of the body, it is more accurate to approach cellulite as an integrative signal, revealing the overall state of the organism. And while it is not possible to completely eliminate all factors (such as hormonal or genetic predisposition), it is possible to act on circulation, stress management, and lifestyle to minimize its visual impact and support overall skin health.
Sources :
- Cellulite: Current Understanding and Treatment – A Gabriel et al. (2023). Oxford University Press / Aesthetic Plastic Surgery Review. PubMed Central.
https://pubmed.ncbi.nlm.nih.gov/37424836/ (PMC) - Cellulite (lipodystrophie). Wikipédia.
https://fr.wikipedia.org/wiki/Cellulite_%28lipodystrophie%29 (Wikipédia) - Open-Label Uncontrolled, Monocentric Study… – A Scarano et al. (2025). MDPI Life.
https://www.mdpi.com/2075-1729/15/7/1148 (MDPI) - Cellulite & Skin Tightening Review of Pathophysiology and Topical Treatment. ResearchGate / Dermatology.
https://www.researchgate.net/publication/387251856_Cellulite_Skin_Tightening_A_Review_of_Pathophysiology_and_Topical_Treatment (researchgate.net) - Cellulite : comprendre ses hormones pour une peau lisse. Aesthe.com (2024). https://aesthe.com/medecine-esthetique-corps/conseils-corps/la-relation-entre-cellulite-et-hormones/ (Aesthé)