Comment les cycles féminins influencent la santé cutanée
How female cycles shape skin health
The skin is not a passive surface or a purely aesthetic envelope. It is a living, responsive organ that constantly reacts to internal biochemical signals. Among the most influential of these signals are hormones, which fluctuate throughout the menstrual cycle and directly affect hydration, sebum production, sensitivity, and overall skin appearance. Understanding skin and female hormonal cycle interactions helps explain why skin rarely looks or feels the same every day of the month—and how to better support it through these changes.
How hormones communicate with the skin
From a biological perspective, the skin expresses hormone receptors and responds actively to endocrine messages. Estrogens, progesterone, and androgens influence the epidermis, dermis, sebaceous glands, and even the skin microbiome.
Estrogen: the skin’s structural ally
Estrogens—particularly estradiol—play a central role in skin quality. Scientific research shows that they:
- Stimulate collagen and elastin synthesis, improving firmness and elasticity
- Enhance skin hydration by supporting lipid and water retention
- Improve microcirculation, contributing to a more even and radiant complexion
When estrogen levels are high, especially just before ovulation, the skin often appears smoother, brighter, and more supple.
Progesterone and androgens: shifting the balance
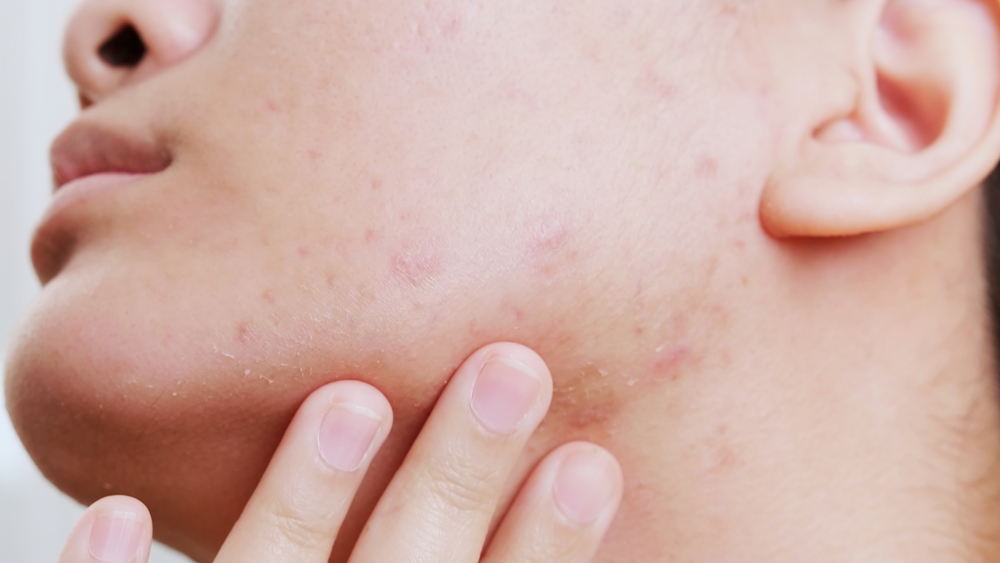
After ovulation, progesterone rises and androgens exert a stronger influence. This hormonal shift stimulates sebaceous gland activity, increasing sebum production. As a result, skin may become oilier and more prone to clogged pores or breakouts.
In cases of hormonal imbalance—such as relative androgen excess—these effects can intensify, contributing to acne or seborrheic skin patterns. Hormonal fluctuations are also known to trigger flare-ups in inflammatory skin conditions like acne, eczema, or psoriasis.
The menstrual cycle: hormonal phases, visible skin changes
The menstrual cycle unfolds as a sequence of hormonal variations, each phase bringing its own skin characteristics.
1. Follicular phase (from menstruation to ovulation)
Estrogen levels gradually rise. During this phase, studies associate higher estrogen with:
- Improved skin elasticity
- Better hydration balance
- More uniform skin tone
For many women, this is when the skin looks its healthiest.
2. Ovulation: peak estrogen, visible glow
Around ovulation, estrogen reaches its highest levels. Increased microcirculation and dermal elasticity may explain the commonly reported “mid-cycle glow.” This phase often coincides with optimal skin resilience.
3. Luteal phase (after ovulation)
Progesterone becomes dominant, stimulating sebaceous activity. Common skin changes include:
- Increased oiliness
- Higher risk of inflammatory blemishes
- Heightened skin reactivity or irritation
This is the phase most associated with premenstrual breakouts.
4. Menstruation: hormonal withdrawal
When both estrogen and progesterone drop, the skin may temporarily feel:
- Drier
- Duller
- More sensitive or reactive
Some women report increased redness or tightness during this phase.
Together, these changes illustrate how closely skin and female hormonal cycle are intertwined.
What science observes in measurable skin parameters
Research has documented cycle-related variations in several skin markers:
- Hydration and barrier function: Transepidermal water loss (TEWL) fluctuates with hormonal changes, reflecting estrogen and progesterone levels.
- Elasticity and blood flow: Skin elasticity and cutaneous circulation tend to peak near ovulation.
- Sensitivity: A significant proportion of women report increased skin sensitivity during the luteal phase or menstruation.
These findings confirm that skin changes are physiological—not imagined.
Beyond the cycle: menopause and long-term hormonal shifts
Hormonal influence on the skin extends beyond reproductive years. During menopause, sustained estrogen decline leads to:
- Thinner, drier skin
- Reduced elasticity and firmness
- Increased wrinkle formation
- Greater skin fragility
Targeted dermatological care and, in some cases, hormonal approaches can help mitigate these effects.
Practical ways to support hormonally responsive skin
1. Track your personal patterns
Observing how your skin changes throughout your cycle helps anticipate needs and adjust care proactively.
2. Use adaptable skincare routines
- Pre-ovulation: light hydration and sun protection
- Luteal phase: oil-balancing and anti-inflammatory ingredients (e.g., niacinamide, salicylic acid)
- Menstruation: soothing, barrier-repair formulas
3. Support skin from within
Balanced nutrition rich in omega-3s, antioxidants, and fiber supports overall skin health.
4. Seek professional advice when needed
Persistent acne, severe sensitivity, or inflammatory conditions warrant dermatological evaluation.
In summary: skin health is hormonally rhythmic
The relationship between the skin and hormones is intimate and cyclical. Recognizing how skin and female hormonal cycle interact is not just a scientific insight—it is a practical tool for better self-care. By listening to these patterns, adapting routines, and respecting the body’s rhythms, skin care becomes more responsive, realistic, and effective.
📚Sources
- The menstrual cycle regularity and skin — NIH PMC — https://pmc.ncbi.nlm.nih.gov/articles/PMC10230734/ (PMC)
- Effect of estrogens on skin aging and the potential role of SERMs — NIH PMC — https://pmc.ncbi.nlm.nih.gov/articles/PMC2685269/ (PMC)
- Physiological Changes in Women’s Skin During the … — PubMed — https://pubmed.ncbi.nlm.nih.gov/39776723/ (PubMed)
- Sensitive skin and the influence of female hormone — PubMed — https://pubmed.ncbi.nlm.nih.gov/27873738/ (PubMed)
- Managing Menopausal Skin Changes: A Narrative Review — NIH PMC — https://pmc.ncbi.nlm.nih.gov/articles/PMC12374573/ (PMC)