Understand, Prevent, and Take Care (Without Taboo!)
A urinary tract infection is often treated like a “small inconvenience,” whispered about between friends , but it is far more than that. It is a real intimate health concern, especially for women, and it occurs with striking frequency: around 60% of women will experience at least one episode in their lifetime. (MDPI)
This complete guide will help you understand what really happens in the body when an infection occurs, why women are more affected, how to recognize the signs, what treatments exist, and most importantly , how to protect yourself from recurrence.
🧠 The Urinary System: What Are We Really Talking About?
Before diving into the details, let’s set the basics.
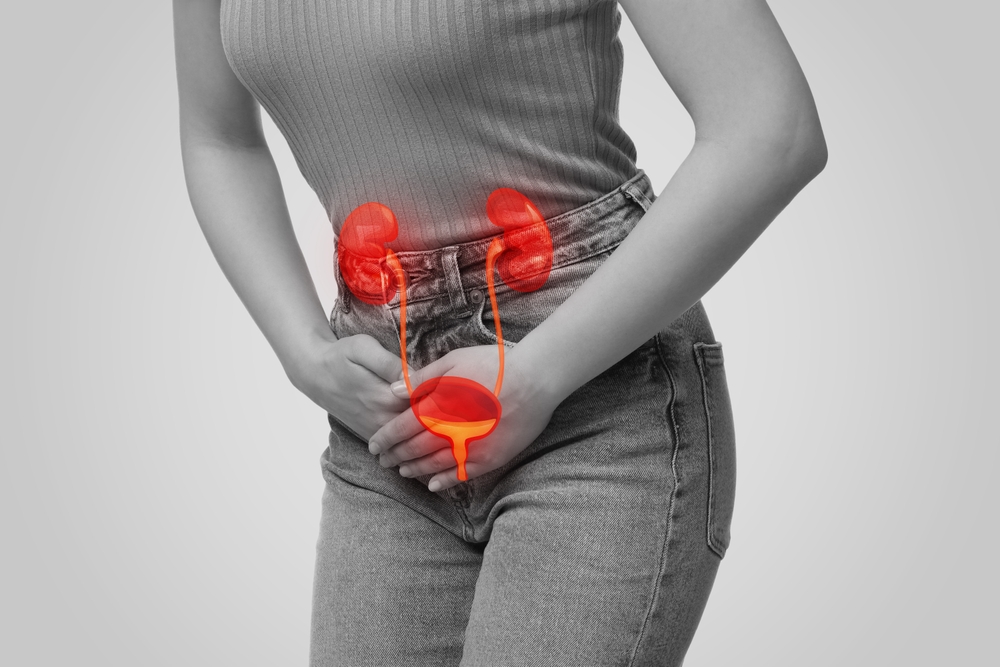
The urinary system is like a transport tunnel for the body’s liquid waste. It includes:
- the kidneys (filter the blood)
- the ureters (carry urine to the bladder)
- the bladder (stores urine)
- the urethra (releases urine outside the body) (Mayo Clinic)
A urinary infection happens when microorganisms , mainly bacteria , colonize part of this system, triggering inflammation and a variety of symptoms. (NCBI)
🦠 Why Are These Infections So Common?
1. Female anatomy
In women, the urethra (the canal through which urine exits) is much shorter than in men. This makes it easier for bacteria from the perineum or digestive tract to reach the bladder. This anatomical difference is a major predisposition factor.
2. Bacteria are everywhere
Most of the time, the main culprit is Escherichia coli, a bacterium naturally found in the digestive tract. Sometimes it ends up where it doesn’t belong and travels up the urethra to the bladder. (PMC)
3. Other risk factors
Several situations increase the risk of infection, including:
- sexual intercourse (especially if hygiene is not optimal)
- certain contraceptives such as spermicides
- hormonal changes (menopause, pregnancy)
- bladder emptying disorders or anatomical abnormalities
- personal history of UTIs
In short: every time bacteria take a “wrong turn,” there is a chance they settle , even though the body is usually well equipped to fight them off.
⚠️ The Different Types of Urinary Infections
Not all urinary infections look the same. Common types include:
🔹 Cystitis (bladder infection)
The most frequent and usually the least serious form. It affects the bladder and causes local inflammation.
🔹 Urethritis
Inflammation of the urethra, sometimes confused with a sexually transmitted infection when discharge or unusual pain is present. (Mayo Clinic)
🔹 Pyelonephritis (kidney infection)
When infection reaches the kidneys, it can become serious: fever, back pain, and overall malaise may occur. This is a medical emergency. (Mayo Clinic)
🔍 Symptoms: How to Recognize Them
Symptoms vary depending on where the infection is located, but some signs are especially common.
📌 Lower infection symptoms (cystitis/urethritis)
- burning when urinating, sometimes described as “stinging with every drop”
- frequent urge to urinate with little urine produced
- cloudy or foul-smelling urine
- pressure or discomfort in the lower abdomen. (Mayo Clinic)
📌 More severe symptoms (kidney infection)
- high fever, chills
- back pain or pain on the side
- nausea or feeling generally unwell.(Mayo Clinic)
In some groups (older adults, very young children), symptoms can be atypical and harder to detect, so vigilance is essential.
🧪 How Is a Urinary Infection Diagnosed?
Diagnosis mainly relies on a urine culture test, which looks for bacteria, white blood cells, and signs of inflammation.
This test confirms the infection and helps guide the most appropriate treatment.
In some cases, a simple urine dipstick test is also used to quickly detect infection markers.
💊 Treatments: When and How?
Most symptomatic infections require antibiotic treatment prescribed by a doctor to prevent progression or recurrence.
Simple cystitis
A short antibiotic course (often 3 to 5 days) is usually enough to eliminate the infection. (NCBI)
Pyelonephritis or severe forms
These may require stronger antibiotics and sometimes intravenous treatment in the hospital..(Mayo Clinic)
It is essential to follow the full prescription even if symptoms disappear quickly, to reduce the risk of antibiotic resistance (JAMA Network)
🛡️ Prevention: Keeping Infection Away
Prevention is often easier than cure, especially for recurrent infections.
💧 Drink enough water
Water plays a key role: increasing urine volume helps flush the urinary tract and limits bacterial adhesion.(Mayo Clinic)
🚻 Gentle intimate hygiene
Soft hygiene without irritating products, and wiping from front to back, can reduce the risk of bacterial “migration.”
🍒 Other strategies (still debated)
Some studies suggest cranberry extracts may reduce bacterial adhesion to urinary walls , but results are not consistent across all clinical trials .(The Australian)
🩺 Special follow-up for at-risk women
Women who experience multiple infections per year may benefit from a personalized prevention plan with a healthcare professional.(JAMA Network)
🔄 What About Recurrent Infections?
If a woman experiences two UTIs or more in six months (or three or more in one year), this is considered recurrent infection.This may require a different approach, including specific advice or preventive treatments.
A recurrent urinary tract infection can also be a sign that risk factors need to be investigated more deeply. (Mayo Clinic)
🎯 Conclusion: An Intimate Topic, But Not a Taboo
Urinary infections are common , especially in women , but they should never be minimized, socially or medically.
Early diagnosis, proper treatment, and simple prevention measures can make a huge difference. And if infections come back too often, it is important to explore personalized strategies with a healthcare professional to regain comfort and peace of mind.
Protecting yourself from urinary tract infection recurrence is not about fear , it’s about knowledge, prevention, and self-care.
📚Sources
- Flores-Mireles AL, et al. Urinary tract infections: epidemiology, mechanisms of infection and treatment options. Nat Rev Microbiol (2015). https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4457377/ (PMC)
- Car J, et al. Urinary tract infections in women: diagnosis and management. BMJ (2006). https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1326933/ (PMC)
- Turcu FL, et al. Recurrent Urinary Tract Infections in Female Patients , A Review. J Clin Med (2025). https://www.mdpi.com/2392-7674/12/1/5 (MDPI)
- Al Lawati H, et al. Urinary Tract Infections: Core Curriculum 2024. Am J Kidney Dis (2024). https://www.ajkd.org/article/S0272-6386%2823%2900837-5/fulltext (AJKD)
- MSD Manuals. Infections bactériennes des voies urinaires. MSD Manual Professional (2022). https://www.msdmanuals.com/fr/professional/troubles-génito-urinaires/infections-urinaires/infections-bactériennes-des-voies-urinaires (MSD Manuals)